Blog
The “Hill of Sorrow” and how getting better can sometimes feel like getting worse…
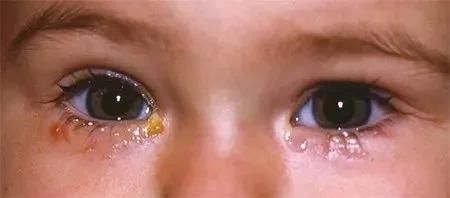
As a dry eye specialist, I can attest that the symptoms of dry eye disease can be wildly variable from patient to patient. The scariest patients are the ones with advanced dry eye disease and related ocular surface diseases, who have little to no symptoms. This is most often related to the slow onset of this often insidious disease. I like the analogy of adding a daily single straw to a camel’s back. From one day to the next, the camel is largely unaware he (or she) is carrying any straw at all - until one day (perhaps from a small stumble - in this analogy - but now think of what a stumble could be to a dry eye - perhaps a little allergy, or minor infection, a surgery, a new glaucoma medication or just staring at a digital screen a little too long), now the camel falls down and can’t get up again. Even worse is when the corneal nerves that serve the surface become slowly damaged from a lack of healthy tears (or other diseases like diabetes or infections like shingles). Now, as the tears get worse and the surface gets drier and more damaged, the eyes actually start to feel “better” because they are getting numb from the damage. These patients may feel worse as we start to improve their tears, and heal their surface and nerves. This can explain why some patients are being told by their doctor that they are getting better even as they feel they are getting worse. Fortunately most will eventually feel better as they get better (this has been dubbed the “Hill of Sorrow” by Dr. White of Sky Vision). The short answer is that dry eye is a complex disease with an equally complex range of findings and symptoms. Best to find a good dry eye specialist and work closely with them until you get better - and then work even harder to stay that way. Caught early, it can be pretty simple to take care of, but caught late it can be a really tough road to fix.
To schedule an appointment with Dr. Jaccoma, call Excellent Vision at either of these two dry eye offices:
(1) 155 Griffin Rd, Portsmouth, NH 03801 (603) 574-2020
(2) 3 Woodland Rd, STE 112 Stoneham, MA 02180 (near Boston) (781) 321-6463
Can I use eye “whiteners” (like Visine or Lumify) when my eyes get red?
As a dry eye specialist, I frequently get questions like this. The simplest answer is “rarely!” Redness is a sign of inflammation (from any of many causes). Inflammation is the body’s response to irritation and will dilate blood vessels so they can deliver larger quantities of the body’s natural defenses to the site of irritation (in this case, the eyes). Anything that make eyes look “whiter” (like regular Visine or the newer drop, Lumify) by causing the big, red blood vessels to constrict (“shrinking them”), will risk “rebound redness” when the little muscles in those blood vessels eventually need to “relax.” Most can get away with this if they’re only using it “once in a blue moon.” Doing this over and over, leads to “addiction,” where skipping the drop makes eyes red, swollen and miserable. The bigger problem is that the more you use the drop, the faster it wears off, requiring more frequent applications and giving less relief. (Think of the rebound issues for those who regularly use nasal decongestants like Afrin). Add to that - the fact that these drops contain preservatives (like BAK) that prevent green, fuzzy stuff from growing in the bottle. Preservatives are toxic chemicals able to kill germs, but also capable of harming tear glands, which can make you progressively more dependent on artificial tear products (since you no longer can make your own). For those already suffering from this addiction, the best recourse is to work with a dry eye specialist who can provide better treatments to address the root cause of the redness (like dry eyes, toxic makeup products, blepharitis and/or allergies) and will sometimes prescribe slow tapers with supportive anti-inflammatories (like low dose steroids) to assist in the recovery. I’ve posted a lot on tears and dry eye treatments. One is available here: https://www.eyethera.com/.../why-cant-i-just-use-some...
What else is new? - A new numbing drop (& how it can help with things like Maskin Probing) and a new “implantable” steroid!
Dextenza is a new implantable steroid. Responding to the question of using Dextenza for relief of dry eye flares – Dextenza is a dissolvable, punctal plug-like device that releases Dexamethasone (a powerful steroid) for up to 30 days before fully dissolving. It has been approved for use in recovery from eye surgeries and for severe eye allergies, but a recent study suggests it may be useful in treating dry eye disease.
Steroids are anti-inflammatory medications that come in differing degrees of strength and are generally coupled with preservatives in drop and ointment forms. The strongest (like Dexamethasone) are capable of shutting down the natural defenses (which are often involved in dry eye issues) – so this can explain the rationale for using them in dry eye, allergy and post-surgical inflammation. I posted on steroids (and anti-inflammation) here: https://www.eyethera.com/blog/segment-10-b-when-we-are-at-war-with-ourselves
As far Dextenza in this setting, all the steroid-related pros and cons relate. The benefit of this device is the slow, continual release, the lack of preservatives, and the fact that it takes daily drops off the table (certainly a convenience factor). The unique negatives include:
- Price (much more expensive than the drops – and since this is considered an “off-label use” it may not be covered by insurance). Check with your provider about cost.
- The “one size fits all” means some that have very small or very large openings to their tear duct may not be a candidate. Certainly, if the puncti (openings to the tear ducts) have been cauterized shut, then it won’t be possible to use it. It also comes in but one strength, so if a little less or a little more would be better, then it might under or over treat.
- It is designed to drop below sight into the tear duct. This leaves the question of whether it might pass directly to the nose (where it won’t help the eye) – and though the company has assured me this is not common (it is designed to swell and “stick” in the tear duct passage near the lid margin), once it “drops in” there is no way to know with certainty where it may land.
- The duration (up to 30 days) is longer than most flares might need (most seem to do OK weaned over 2 weeks, but some do need longer) – and when it comes to strong steroids, less is often better. Eysuvis was approved for dry eye flares because it is a very dilute form of Loteprednol (a weaker steroid to begin with) – so this is more my usual “go-to.” This is a link to the dry eye drug study: https://www.ophthalmologytimes.com/view/ocular-therapeutix-announces-topline-results-for-phase-2-clinical-trial-of-otx-ded-for-short-term-treatment-of-dry-eye-disease?fbclid=IwAR1ZRI5QsteFgQAC07YfAmerlYOcqYNFvAdMDcn06VFQHzJSEURGq-TAzDk and it is no surprise that, according to the study report: “The most common ocular adverse events for subjects treated with OTX-DED (Dextenza insert) were epiphora (lacrimation increase) (8.1%) and elevated intraocular pressure (IOP) (3.6%).” Epiphora is tearing (commonly reported as flowing down the cheek) and this would be a common side effect of a punctal plug (blocking the tears from flowing down the natural tear duct pathway to the nose) where elevated eye pressure can eventually lead to nerve damage called Glaucoma – see my blog on punctal plugs and “Toxic Soup,” here: https://www.eyethera.com/blog/what-about-punctal-plugs-or-why-not-dam-up-those-damn-tears and https://www.eyethera.com/blog/when-tears-dont-drain-properly-you-get-toxic-soup-and-the-toxic-soup-syndrome
My added concern is that when a “toxic soup” situation exists, this will cause an apparent dry eye flare. Adding a steroid into the toxic soup may quite the eye, but does not relieve the obstruction causing the toxic soup. Rather, it may add further obstruction to it. It also may knock out the immune system’s ability to defend against germs that may brew in this soup, so I don’t see Dextenza as a particularly good fit for many - but may be a specialty-specific tool to help select patients. As always, check with your dry eye specialist to see if you may qualify for its use.
Responding to a question of Maskin style probing without using topical anesthetics or IPL (due to extreme sensitivities to preservatives in most drops, gels and sensitivities to all forms of heat - including IPL, as is common among many with Rosacea-related dry eye) – I posted the following:
I've posted on a lot of dry eye care but your question is a new one (I have yet to have any patient ask to forego all topical anesthetics, but do routinely offer small injections of numbing medication to add a deeper level of numbing as probing can otherwise be relatively painful) - and the short answer to tolerating the numbing vs tolerating the treatments (without the numbing) - is that it almost always is necessary to do some numbing with drops or gels prior to Maskin Probing (or any number of other dry eye treatments). We do have a new, preservative free gel (IHEEZO) more commonly used for cataract surgery (it offers a deep level of topical anesthesia without the irritating preservatives found in most other topical anesthetics), so this might help in cases like yours. In my Maskin protocol (a bit different from each doctor), I start with putting metal eye shields in each eye (sometimes over a bandage contact lens for patients with your complaints), which could be uncomfortable without some numbing, followed by IPL over the lids (to soften some oils and "wake up" some glands). I follow this with a strong scuffing of the lid margins (to remove any gummy/waxy "plaque" and then probe serially using a high powered operating microscope, as deep as the MGs will let me (trying for 4mm i upper and lower lids). I follow this with removing the metal shields, applying a plastic shield and then heating with Radio Frequency to "melt" any residual waxy oils and then expressing all of the probed glands while they are optimally "hot." This attempts to purge any "bad" oils and leave room for better oils to come along. I have patients apply a combination antibiotic and steroid eye drop on a tapering schedule to prevent germs from getting a foothold in the probed glands and preventing scar tissue from recurring in the probed areas, so the glands can continue to do their best (& hopefully regenerate to their fullest potential). Sticking to this protocol has helped most of my patients to achieve the highest level outcome - based on a decade of doing the probing along various other protocols and using a variety of other tools. I find some basic "homework" (taking good Omega oils, doing good lid hygiene and, when appropriate, some home-based heated eyelid crunches to help turn over oils) along with a series of IPL and heated expressions, can often help enough (when caught early) to prevent the need for the probing - and when probing is required, to help "wake-up" and support the glands, so that probing can better succeed. Following this, the same ongoing homework and some degree of maintenance treatments (customized to the patient's needs) is typically needed. Check out my blog at eyethera.com for more on my typical "homework" and to see me perform some of these peripheral treatments. An earlier post on Maskin probing can be found here: https://www.eyethera.com/blog/why-do-expensive-dry-eye-treatments-fail-and-what-is-maskin-probing
I hope this helps!
To schedule an appointment with Dr. Jaccoma, call Excellent Vision at either of these two dry eye offices:
(1) 155 Griffin Rd, Portsmouth, NH 03801 (603) 574-2020
(2) 3 Woodland Rd, STE 112 Stoneham, MA 02180 (near Boston) (781) 321-6463
Are there any new eye drops for dry eye?
In a word, YES: The pipeline is robust and we have a few new options recently USFDA approved and likely soon available. My “take” on them, based on their published studies and some discussions with colleagues involved in some of the studies (as well as some with a few years experience with Miebo, abroad).
Perflorohexyloctane (Miebo): Novaliq introduced this as EyeSol, then marketed it in Europe as EvoTears or Hycosan Shield, and now in the USA as Miebo by B&L,. It is 100% water-free , preservative free oil, dispensed as an “ARTIFICIAL TEAR” that may take the place of the normal human oil to help seal in the moisture when normal oil is missing. It has been used as a carrier for Cyclosporine (see the piece on Vevye, below, where they refer to Miebo as an “excipient” – in this case, meaning carrier), so could become useful in adding a measure of better tolerance to the stinging many patients complain about with the standard forms of Cyclosporine already available and appears to have a faster onset of action, though I don't know of any head-to-head studies between Vevye and Restasis, Cequa or the other cyclosporine eye drops already available. (chemically F6H8, Miebo is in the family of semifluorinated alkanes. I think of Miebo as “Tear Teflon,” as Teflon is in the family of Per- and polyfluoroalkyl substances).
My concerns about this product include the following: (1) the studies that got Miebo approved only compared it to dilute salty water (a pretty low bar), so how it will compare to other artificial tears already out there is a matter of debate. (2) Like any other preservative free artificial tear, I worry that if it "works," it is at best a better "Band-Aid" - in that it may allow patients yet another opportunity to treat symptoms (and feel better) without addressing the issues causing the symptoms (the underlying disease). This may "kick the can down the road" enough that the disease can progress to a point where it becomes ultimately harder to ever fix - and I can't see an inert chemical truly doing all the good things a normal, healthy, human tear would do for the surface of the eye.
That. being said, I've heard rumors and innuendos that it may "dissolve" some of the waxy oils clogging the oil glands. If so, I may have to retract this concern, as that could help "fix" the MGD problem - but until I see good clinical evidence of this, I remain a skeptic. (3) Not being a chemist, I may be off base, but this chemical seems a bit close to the "forever chemicals" (like Teflon derivatives) that I've tried to avoid in my lifetime. Things that are not intrinsic to human biology, nor easily broken down and digested, seem to have a habit of doing bad things. I understand that this has been used for years abroad and passed strict clinical trial evaluating safety, so I hope these fears remain unfounded. I should add that while sold in Europe for years, it has not been what most of my European colleagues would call a “game changer” for their dry eye patients. So far, it appears to be yet another artificial tear product that helps some more than others in fending off dry eye symptoms – so my expectations remain rather low (Vevye may be a different matter if it truly proves a better way for delivering cyclosporin - a medication I’ve come to know and respect – I’ll keep you posted).
Reproxalap: developed by Aldeyra (a so-called RASP inhibitor, referring to its mechanism of inhibiting a common part of the inflammation pathway leading to allergic responses and inflammatory reactions that can lead to dry eye disease) - I think of it a bit like a steroid without the side effects of stirring up eye pressure (IOP) that could lead to - or aggravate glaucoma, nor the side effect of aggravating or causing cataracts. This by itself is a major advancement in the field of anti-inflammation and may add a new chapter to what we can offer to fight inflammations causing redness, aqueous tear deficiency (what otherwise is treated with Cyclosporine or Lifitegrast, unless a steroid is used) and the many nuanced inflammations relating to allergies, friction, evaporation, etc. The place it will not likely be helpful is when fighting germs. Since it can be tough to determine when redness relates to an infection (or germ-related problems like blepharitis), versus the many other dry eye and allergy related issues causing redness, we may still need to be cautious about indiscriminate use - and like all new medications, it may take us a while to determine the best uses for this new class of drug.
To stay fair to the industry developing this new form of cyclosporine - I’ve copied verbatim, an introductory report directed to eye doctors (still pretty readable for the non-physicians who like to read frontline information)…
Taken from: Glance by Eyes On Eyecare <glance@eyesoneyecare.com>
“Are there any new eye drops for dry eye?
Yes! Novaliq GmbH has received FDA approval for VEVYE (cyclosporine ophthalmic solution) 0.1%, indicated for the treatment of the signs and symptoms of dry eye disease (DED).
Tell me more about VEVYE.
Developed under the name CyclASol, VEVYE is a cyclosporine formulation solubilized in a novel, water-free excipient—with no antimicrobial preservatives, oils, or surfactants.
Talk about this water-free component.
VEVYE is formulated with EyeSol, Novaliq’s proprietary, preservative- and water-free technology that uses ultrapure semifluorinated alkanes (SFAs).
According to the company, these SFAs have very low surface tension and viscosity, dispense low-volume drops (<12 µL) that do not stimulate blinking or reflex tearing, and have the same refractive index as water.
And this helps because…
By having low surface and interface tension, the drops are able to spread rapidly over the ocular surface and form a flat, transparent layer that could allow for improved visual clarity—without potential blurring.
What’s the dosing?
Per its prescribing information, one drop of VEVYE can be instilled twice a day (BID) in each eye, approximately 12 hours apart. See here for the full details.
What makes this unique?
After drops are administered, VEVYE can exhibit an increased residual time on the ocular surface and allow for a high bio-availability within the target tissues to release the solution’s fast onset of action within 2 weeks.
Any clinical trial info?
Yes! The randomized, multicenter phase 2/3 ESSENCE-1 trial and phase 3 ESSENCE-2 trial both concluded that the use of VEVYE (then CyclASol) led to clinically meaningful early therapeutic effects on the ocular surface when compared to vehicle. And the multicenter 12-month safety extension trial (ESSENCE-2 OLE) confirmed the effects of CyclASol were maintained and, in some cases, even improved for most sign and symptom endpoints.
Significance?
With this approval, VEVYE is now the first and only cyclosporine solution indicated for the treatment of signs and symptoms of DED, with an efficacy demonstrated over 4 weeks.
What else to know?
This latest approval marks the second for Novaliq is less than a month: the company, in partnership with Bausch + Lomb, received FDA approval in May 2023 for MIEBO (perfluorohexyloctane ophthalmic solution) for the treatment of signs and symptoms associated with DED. Click here for the details.”
Stay tuned!
Do results of IPL treatment vary by technique and by the filters used? (& does it regenerate withered glands?)
Do results of IPL treatment vary by technique and by the filters used?
I often get asked this question as patients may find me after getting multiple treatments elsewhere and they wonder if my treatments will be different. I have a lot of older, relevant posts on IPL for dry eye treatment, including this one: https://www.eyethera.com/blog/more-on-ipl but will add some updated information and share some thoughts below.
The short answer is yes and yes. In fact, not all IPL technology is the same, either. The two types of IPL are “Broad Band” (BB) vs “Selective Filtering.” (SF) Major companies have good reasons to produce one or the other, as each has strengths and weaknesses. The strength of BB is that a broad range of light energies will accomplish a broad range of treatment - mostly tailored towards aesthetic purposes, when a single pulse of BB will affect pigment (irregularities of skin color is referred to as dyschromia and can make skin appear older - like age spots - and therefore appear less attractive, as well as affecting vascular issues or hair reduction, all at the same time. Dr. Steve Mulholland refers to this as the “grenade effect.” The SF type of IPL uses a narrow (as opposed to broad) range of light by employing a very selective filter. This can approximate the effect of a laser, which is all of one “color” (or wavelength). Dr. Mulholland refers to this as a “sniper” that can knock out a single target. In the world of dry eyes, there are specific targets that appear to be most related, so the SF IPLs are tailored to that treatment. While BB IPL can cover the same wavelengths, using multiple wavelengths can be like using a sledgehammer when a smaller hammer would do. Assuming different doctors use the exact same machine, results can vary. (SF IPL is what Lumenis was able to convince the FDA as being safe and effective for dry eye treatment, so is the type used by myself and, I believe by Dr. Periman, though I should also add, after getting FDA clearance, Lumenis has since developed a smaller handpiece that they call Optilight and claims it can treat around eyes more precisely). Understanding how light works to treat different types of skin and eye conditions is as important as the equipment used. Treating ocular rosacea (a common form of dry eye disease) means treating abnormal blood vessels. Too much pressure on the handpiece can compress the blood vessels and make them less visible to the light (so affecting them less). Tipping the handpiece at an angle can scatter the light, making it less effective. Cooling the skin too much can also shrink the vessels (like compression does), but not enough cooling can be uncomfortable for the patient and may result in surface burns. I could go on and on, but the key is to understand that Drs like Dr. Periman (and Dr. Toyos, who pioneered/invented IPL for this treatment) literally wrote the book on much of this, so I think her patients can expect the highest levels of care (apart from her being an excellent doctor). So, the equipment, the technique and the filters all are important parts of the equation. THIS IS NOT TO SAY THAT THERE ARE NO OTHER QUALIFIED DOCTORS (& related staff) WHO CAN PROVIDE EXCELLENT CARE. Many have been trained and/or influenced by Dr. Periman and/or Dr. Toyos (I’ll count myself as lucky among them) and some come from other walks of careers that might bring other talents to their practice (I like to count myself in this boat as well, having used dermatology lasers to treat skin for aesthetic purposes for many years as well as pioneering/inventing RF for dry eye care). In general, those practitioners have gone out of their way to get better training and experience than the average professional, so don’t be afraid to ask questions about their experience. All should have a minimum of a day of training from a nurse representative of the company making the IPL, but may will have taken extra courses and/or spent time with leaders (like Dr. Periman and Dr. Toyos) who have shared their knowledge and best practices with them.
Second: Does IPL regenerate withered Meibomian Glands?
Numerous reports (many anecdotal) show visible improvement in these critical glands with repeated treatments over time. There are several problems when it comes to clearly documenting visible improvements.
1) the technology for imaging is prone to errors as the angle and degree of light, rotation of the lid and focus will all affect how the glands are perceived.
2) it typically takes years for glands to “go bad” and years to see them “go good.”
3) infrared cameras tend to capture the “active” portions of the glands. As the glands become more active, they can appear to “regenerate.” How much actually regenerates is a matter of some debate. However, many of us are finding this for many of our patients. At least one clinical study found this likely to be true…
– excerpted from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6802620/
“Yin and collaborators analyzed the effect of IPL on two indexes describing the meibomian gland microstructure: the acinar longest diameter and the acinar unit density. Both these parameters showed a significant improvement after treatment.27 Authors speculated that the changes in gland microstructure were induced by the photomodulation effect of IPL on acinar cell activity.27” (Incidentally, this article has a good review of the use of IPL in dry eye treatments, ut shies away from use directly over lids - which is a common part of the “Periman Protocol” that I and many other IPL practitioners find most helpful to our patients - and involves use of expensive metal eye shields under the lids, to effectively protect the eyes during the treatment).
Fortunately, following the gland function is usually easier to monitor than their anatomy (Tear Break Up Time, results of expression at the slit lamp (amount and quality), Tear Osmolarity are all useful tools in evaluating improvement). Ultimately the subjective dry eye questionnaires (SPEED, OSDI, etc) may give a good clue, too, as they allow the patient to indicate to us the type and amount of improvement they sense as a result of the treatments.
Manuka Honey - How sweet it is (or might be?) for treating dry eyes!
Have you heard of Manuka Honey? Until relatively recently, I had not – but a series of postings in various dry eye forums brought it into focus for me (pun intended). I’ve since learned that it’s a form of honey currently being used to treat a variety of medical issues, from burn and superficial wound care to dental/gum and throat issues, to my favorite topic – blepharitis, dry eyes and ocular surface diseases. It is created from the nectar of Manuka bush (leptospermum scoparium) flowers by unique species of bees (while there are 28 species of bees in native New Zealand, it is said that only one is shared with Australia, which by itself, has over 1,500 species of bees and both countries grow Manuka plants producing this honey).
Manuka is also called a “tea tree” but differs from the tea tree we think of (Melaleuca Alternifolia) when we think of “tea tree oil.” Both types of tea trees are from the myrtle family of shrubs (and can grow into trees) but Mauka has found a niche for its honey, while the “other tea tree” found its niche for its oil. (Not to confuse further, but Manuka can also be distilled for its oil, which is touted for its medicinal benefits in topical treatments but is less pungent than the “other” tea tree oil).
The "Man of Bicorp" holding onto lianas to gather honey from a beehive as depicted on an 8000-year-old cave painting near Valencia, Spain https://en.wikipedia.org/wiki/Cuevas_de_la_Ara%C3%B1a#/media/File:Cueva_arana.svg
Honey and mankind go back untold millennia, with early cave paintings suggesting we gathered it at least 8,000 years ago (see above), but ancient Egyptians (circa 3,500 BCE, https://bugsinourbackyard.org/the-fascinating-history-of-honey/ ) recorded “a large number of practical applications for honey. Citizens used the liquid as a sweetener in food, while doctors capitalized on the natural antibiotic properties of honey to produce salves for healing wounds. Even the mummified benefited from Egypt’s expert use of honey, as many of their sarcophagi were sealed with wax collected from honey producing hives and full honeypots were typically offed to the dead as food during the afterlife. Believe it or not, some mummies were even embalmed in the golden liquid to improve preservation of the body!”
Webmd has a very good article on Manuka Honey, which I will clip and paste in near total, from here:
https://www.webmd.com/a-to-z-guides/manuka-honey-medicinal-uses
They claim: “It wasn't until the late 19th century that researchers discovered that honey has natural antibacterial qualities.
Honey protects the body against damage caused by bacteria. Some honeys also boost production of special cells that can repair tissue damaged by infection. Manuka honey has an anti-inflammatory action that can help ease pain and inflammation.
However, not all honey is the same. The antibacterial quality of honey depends on the type of honey as well as when and how it's harvested. Some kinds may be 100 times more potent than others.
Components of Manuka Honey
Hydrogen peroxide gives most honey its antibiotic quality. But some types, including Manuka honey, also have unique antibacterial qualities. One of the major antibacterial components of Manuka honey is a compound called methylglyoxal (MGO). MGO comes from the conversion of another compound in Manuka honey known as dihydroxyacetone (DHA), a high concentration of which is found in the nectar of Manuka flowers.
The higher the concentration of MGO, the stronger the antibacterial effect. Honey producers have a scale for rating the potency of Manuka honey. The rating is called UMFTM, which stands for Unique Manuka Factor.
The UMFTM rating reflects the concentration of 3 signature compounds found in genuine Manuka honey, MGO, DHA and leptosperin. To be considered potent enough to be therapeutic, Manuka honey needs a minimum rating of UMF™ 10+. However, doctors and researchers aren’t sure if this rating means anything from a medical standpoint.
How Manuka Honey Is Used
The main medical use for Manuka honey is for wound and burn healing. It is generally used for treating minor wounds and burns. Research shows Manuka honey to be effective in treating other conditions, including:
Skin care including eczema and dermatitis
Soothing a cough or sore throat
Digestive Health
But the evidence is limited on whether it works for these conditions.
The honey used to treat wounds is a medical-grade honey. It is specially sterilized and prepared as a dressing. So the jar of Manuka honey in the pantry shouldn’t be part of your first aid kit. Wounds and infections should be seen and treated by a health care professional.” (My bold italic underlining). I should add that I’d say the same regarding use in and around eyes.
More from Webmd:
“What the Science Says About Manuka Honey
Several recent studies show Manuka honey can be helpful when it’s used on top of wounds and leg ulcers. Studies also show it might fight infection and boost healing.
The Natural Medicines Comprehensive Database lists honey as being "possibly effective" to treat burns and wounds. The Cochrane Review notes that honey may shorten healing times in mild burns and surgical wounds compared with traditional dressings. But they also say more research needs to be done.
Another study suggests that Manuka honey may help prevent gingivitis and other periodontal disease by reducing the buildup of plaque. In some studies, Manuka honey seemed to help prevent inflammation in the esophagus caused by radiation and chemotherapy used for cancer.
Another possible benefit of honey is that, unlike antibiotics, it doesn’t appear to lead to resistant bacteria. These so-called "superbugs" develop after repeated exposure to common antibiotics. Special antibiotics are needed to treat them.
Most of the studies on Manuka honey have been with small numbers of people, and so far, research hasn’t shown that Manuka honey helps with high cholesterol or balancing the bacteria in the gut. Furthermore, no major studies have looked at the effect of Manuka honey on cancer, diabetes, or fungal infections.
Possible Side Effects of Manuka Honey
These may include:
Allergic reaction, especially in people who are allergic to bees
A rise in blood sugar if large quantities are consumed
Effects on certain chemotherapy drugs and interactions with various other medicines.”
This brings up the question of how we might use it to treat eyes and eyelids.
Dr. Rolando Toyos posted on use of Manuka honey products for treatment of eye allergies and for dry eyes here: https://toyosclinic.com/blog-feed/optimel-manuka-honey-drops-a-great-option-for-allergy-eyes-and-allergy-with-dry-eyes It appears his centers may be studying it for the allergy application, but to date, I am not aware of any published clinical studies specifically tailored for eye allergy treatment. Still, Dr. Toyos makes a good case for the anti-inflammatory benefits being useful in this capacity and several small studies suggest it can help for certain skin and nasal allergies.
The following testimonial was posted by a dry eye sufferer, who uses “the drop form for keratitis, the gel form for MGD.” The person posting claims to use:
"a match-head sized drop spread on the lower lid margin. It will sting and the eyes will close automatically. Use gel once a day at night. The drops used 1-4 times a day in addition to any other drops."
Others have complained of the burning and stinging immediately following the application of the gel. My response was: “While I've heard that edible honey has been found in the tombs of ancient pharaohs, indicating the degree to which it may resist bacterial degradation, and where I've read articles reporting studies of (in total) several hundred patients who have tried this as a treatment for dry eye disease, I don't have any personal experience with it in my own patients as of yet. I believe the acidic nature of the product is what gives it the natural antibacterial properties, but this same acidity will typically cause stinging and burning on instillation. My general inclination is that too much stinging and burning may trigger inflammation (the body's reaction to irritation) - and though early reports suggest this unique honey may reduce inflammation (as any antibacterial seems to do), because each patient is different, there are likely patients at either end of the spectrum where some will get positive results and others may get negative results. If you are finding it hard to tolerate, then it seems possible you may be in the latter group - but as I always suggest, it is best to consult directly with your own dry eye specialist to find what may be best for you.”
So, is Manuka (or any other) Honey worth using as a dry eye treatment? I’d say the jury is still out on this, but it does appear to be worth considering. A review of the literature suggests we are still constrained by small studies (so far, 300’s-400’s of patients and not the thousands we expect to see in prescriptive medical trials). Looked at through the lens of antiquity, we definitely have a long history of using honeys for medicinal uses – so one might infer that the staying power over this passage of time is perhaps the best testimonial - but eyes are delicate and special – so before I broadly recommend Optimel (or other honey) products, I’ll be looking within my practice and to future studies to better determine who, when and for what conditions I will recommend them. I also won’t go out of my way to discourage my patients from trying them (and hopefully I’ll be able to track their progress to gain more insights into this medical mystery).
Can eye drops kill you? Part 2: avoiding “Buyer’s Remorse.”
We’ve all heard the term: “Buyer Beware” - though in the world of health safety and in particular, eye safety, should a buyer have to beware? The short answer is “maybe.” I hope by choosing your dry eye specialist with care, we can help eliminate “Buyer’s Remorse.”
Regener-Eyes has been marketed as a “biologic” artificial tear, said to contain some of the proteins and materials found in a pregnant womb. Another company, M2 Biologics followed suite, creating StimulEyes. Regener-Eyes makes a “prescriptive” (or “Pro”) strength (said to require an actual prescription to purchase and requiring refrigeration after opening) and a “Lite” version (said to not require refrigeration and said to not have preservatives). These companies came under the scrutiny of the FDA as unapproved for any treatment – though Regener-Eyes claims to have been approved by the FDA as an Over-The-Counter (OTC) product deemed “generally safe and effective for its intended use.” Upon further research, there is an FDA online service noting the ingredient in the Regener-Eyes product is “Glycerin,” which I will note is not considered a biologic and can be found in other OTC artificial tears (in a very dilute concentration). Whether any of these products contain a biological agent remains a mystery, as the companies have so far refused to clarify what else is in them. I should note that at present, I am unaware of any poor outcomes associated with the use of any Regener-Eyes or StimulEyes products. Because of the lack of preservative (or refrigeration) in a simple dispensing bottle, I found the risk of recommending these products to be too close to the range of problems caused by the drops I covered in my last post and will repost an article I found that helps underscore these risks, along with a simple diagram of unapproved vs approved dispensing bottles for artificial tears (and other eye drops), here:
“Dry Eye Foundation continues to warn against the use of unverified and unsafe eye drops
May 12, 2023
From ingredients that should not be included to ingredients that should be but are not, and improper storage and manufacturing, numerous eye drops have raised safety concerns.
(Image Credit: AdobeStock/Geparda)
The Dry Eye Foundation is warning against the use of certain eye drops marketed for use in the United States.
From ingredients that should not be included to ingredients that should be but are not, and improper storage and manufacturing, Sandra Brown, MD, Dry Eye Foundation board member and medical advisor, has been sounding the alarm since the beginning of 2022.
In April 2022, the Dry Eye Foundation alerted the FDA to 2 brands of unapproved biologic eye drops being distributed commercially as prescription drugs.
“We've been banging this drum since first quarter, early second quarter of 2022,” Brown said. “The exact safety issue is that you cannot put a multidose eye drop that does not contain preservative in a bottle.”
Brown explained the reasoning behind this sentiment, in that preservative-free eye drops need to be put into a bottle specifically designed for them.
“Recently, thankfully, they've developed a special type of dropper that can be used with preservative-free eyedrops,” she said. “You can usually, easily, identify the bottle because it’s got kind of a funny sort of square cap on it [and] is called a multi-dose preservative-free dropper, an MDPF dropper. You cannot take a non-preserved eye drop and put it in a standard bottle. Because it does not prevent backwash.”
Brown described backwash as when the tip of the dropper becomes contaminated, then you let go of the squeeze, the bottle sucks contaminated liquid back into the bottle.
This is one of the reasons preservative-free bottles cannot be put into ordinary bottles, as ordinary bottles do not protect against backwash, according to Brown.
The Dry Eye Foundation includes a list of products that it has concern over on its website. Currently, there are more than 30 brands and even more products that the foundation has listed as an “orange level alert.”
(Image Courtesy Dry Eye Foundation)
The foundation defines an “orange level alert” by the potential for non-sterility of the eye drops because it is an unregistered or unlisted drug, or it is registered or listed, but has red flags. For instance, eye drops that are registered with the FDA contain ingredients not permitted in OTC eye drops or not recognized as preservatives. While some are packaged in conventional multi-dose bottles despite being preservative-free. Which was an issue seen with EzriCare eye drops.
EzriCare eye drops are included in the foundation's “red alerts” which are CDC Health Alerts, FDA Public Safety Notifications, and Class 1 Recalls pertaining to over-the-counter eye drops.
EzriCare eye drops are a product from Global Pharma Healthcare, where an FDA inspection found dozens of contamination issues in a facility in India.
These eye drops were responsible for an outbreak of VIM-GES-CRPA, a rare strain of extensively drug-resistant Pseudomonas aeruginosa, which has not before been identified in the US according to the CDC.
Brown stressed the importance of the unique genetic signature of this strain.
“That's the key thing is that it has a unique genetic signature. and the fact that it's caused serious infection in people from one end of the country to the other, and it has a unique genetic signature means it came over on the boat,” said Brown. “So yes, it's a problem that it was a standard eye drop bottle with no preservative, but it also was contaminated during manufacture … one of the things that [preservatives] are supposed to be able to kill [are] pseudomonas.
You can view a complete list of the alerts and products to be wary of online.
Brown listed some of the ingredients to look out for; “Anything that says, ‘contains vitamins, MSN, amino acids, honey.’ Those are common ingredients that are not allowed in an over-the-counter eyedrops.”
The ease of purchasing eye drops online thanks to websites like Amazon are a greater reason for concern and awareness, said Brown. Consumers need to be sure to “know your seller” when purchasing online.
“It is a buy-at-your-own-risk kind of approach. It allows these products to reach a really wide audience. So, before Amazon took the entry care listing down, it had close to 2500 reviews with a 4.5 star review,” said Brown.
To be safe on purchases, Brown encourages using DailyMed to verify the product.
“What I do say is step one, go to DailyMed, if It's not listed on DailyMed, do not buy it,” she said. “But understand that just being listed on DailyMed, does not mean it's alright.”
Becoming educated on the process of FDA protocols and the ingredients that are included in the products that are being purchased and used are one of the most important acts of self-awareness according to Brown.
“I think my message to ophthalmologists is that EzriCare has taught us that we have to pay more attention to our patients over the counter products,” Brown concluded. “It is time to start looking at them. So have the patients bring them in, dump out their bottles. Check to be sure
they are not using something weird, or, you know, some off-price brand. Especially if the patient's having some strange problem you cannot get on top of, consider whether or not it is actually their over-the-counter products.””
Another journalist reported on the so-called biologic drops here: This is a MedPage Today story.
https://abcnews.go.com/Health/wary-unproven-eye-drop-treatment-amniotic-fluid-fda/story?id=98836159
“Be wary of unproven eye drop treatment with amniotic fluid, FDA says
The FDA says there is no assurance the products are safe or effective.
By Kristina Fiore | MedPage Today
FDA issues warning over amniotic fluid eye drops
The Food and Drug Administration has pushed for regulation around the marketing and sale of birth tissue-derived stem cell products for dry eye disease.
In its ongoing battle against companies selling unapproved stem cell products, the FDA issued a safety communication earlier this month about amniotic fluid eye drops being improperly marketed for dry eye disease.
The communication links to earlier letters to two manufacturers -- makers of Regener-Eyes and StimulEyes -- warning that the products would need an approved Biologics License Application (BLA) to stay on the market, or health care providers would need an investigational new drug (IND) application to deliver them to patients.
"There are no assurances that the products are safe and effective for any disease or condition," FDA said in its safety communication, adding that there are "currently no FDA-approved amniotic fluid eyedrops to treat, mitigate, or cure eye diseases or conditions."
MORE: Death toll linked to contaminated eye drops rising as more report vision loss
Both products appear to be readily available for sale on the internet, with plenty of options on Google Shopping. Although StimulEyes maker M2 Biologics states on its homepage that online ordering of the product is currently unavailable, the product appears to be available for purchase through other channels.
Neither Regener-Eyes CEO Dr. Randall Harrell nor M2 Biologics returned a request for comment.
It's not clear if the companies made other changes to their products or their marketing following the FDA's earlier letters. The original "untitled" letter to Harrell and Regener-Eyes from October said the company made claims on its website that it was a "biological product" composed of "placental-derived biomaterials" and used for the treatment of dry eye disease.
The untitled letter to M2 Biologics sent in November said its website claimed StimulEyes was a "regenerative medicine" product also used for treatment of dry eye disease.
In both cases, the FDA said the products appeared to be a drug and a biological product and would need a valid biologics license to be marketed.
"Your product is not the subject of an approved biologics license application (BLA), nor is there an IND in effect for your product," the FDA stated in both letters.
The FDA has been getting tougher on "birth tissue" companies, which market products that allegedly contain stem cells and other biological materials that are derived from the placenta and umbilical cord. The agency has argued that these are biological products that need to be regulated as such.
Leigh Turner, executive director of the bioethics program at the University of California Irvine, who has long been tracking stem cell companies, said that while "hundreds" of businesses sell such allogeneic birth tissue-derived stem cell products, a "much smaller number of companies advertise purported 'regenerative' amniotic fluid eye drops for dry eye disease and other indications."
"The problem with such commercial activity is that such companies haven't tested their products in controlled clinical trials and the safety and efficacy of such amniotic fluid products in the treatment of individuals with dry eye disease and other diseases have not yet been established," Turner told MedPage Today. "These untested or inadequately tested products pose risks to patients, as the recent public safety notification issued by the FDA notes."
In its letter to Regener-Eyes, FDA noted the company described its product as an "acellular" biological product, meaning it does not contain stem cells, Turner said, adding that it's "not clear what businesses are claiming when they assert such products have regenerative properties."
"It appears to be another example of using the hype and buzz associated with regenerative medicine to sell purported treatments," Turner said.
Paul Knoepfler, of the University of California Davis, who has also been tracking the stem cell industry, said that these products still could contain growth factors and other substances that could have activity in the eyes.
"The drops likely contain hundreds of different fetal proteins and other substances, which don't necessary just do helpful things, so there are definite risks," he told MedPage Today.
He warned that such possible tissue changes "may not be entirely reversible after stopping the drops. We just don't know."
Knoepfler added that any drug placed into the eye could end up "in systemic circulation so there could be risks outside of the eye. I'd also worry about risks of infection."
"There are good reasons to treat these products as drugs and require robust clinical trial data before marketing," he said.
Turner noted the FDA's use of untitled letters to the two companies may not have enough teeth to force any real change, especially as the products appear to be readily available for purchase online.
"More robust regulatory responses are likely needed to curtail such activity," he said.
In its notice, FDA said health care providers should report any adverse events associated with amniotic fluid eye drops to its MedWatch program.”
To schedule an appointment with Dr. Jaccoma, call Excellent Vision at either of these two dry eye offices:
(1) 155 Griffin Rd, Portsmouth, NH 03801 (603) 574-2020
(2) 3 Woodland Rd, STE 112 Stoneham, MA 02180 (near Boston) (781) 321-6463
Can eye drops kill you? Part 1:
In a word, yes.
From some prescriptive drops with built-in risk factors doctors must weigh when prescribing them (like Timolol - used to treat glaucoma - that can stop a heart when you have certain heart issues), to any drop if you have an extreme allergy to something in the drop – there have been scattered, few reports of issues like these - which can lead to severe reactions and even death. More recently, some preservative free artificial tears and an ointment have been found to harbor horribly invasive bacteria that are uniquely resistant to nearly every antibiotic in clinical use. This germ has blinded – and yes – has killed some people unfortunate enough to have used them over the past year.
I posted an FDA alert on this issue several months ago – but at that time, there was still some confusion about which products might be involved and what allowed this problem to happen. Recent information has been published in eye journals, which I can share here:
From - https://theophthalmologist.com/business-profession/eyedrop-out-of-sight
(Eye)Drop Out of Sight
What led to the recent bacterial outbreak in the USA that infected 68 and resulted in the death of three patients?
Jed Boye | 05/11/2023 | 4 min read | Discussion
“Some Big Pharma conspiracy theories revolve around the idea that large corporations operate nefariously, giving patients medications that are actively harmful. Although most such claims are baseless and founded on bogus (or zero) science, there are times when – through negligence, human error, or other unexpected factors – medications can do more harm than good.
In March 2023, the USA saw the peak of an outbreak of a rare, drug resistant strain of Pseudomonas aeruginosa (1) – a bacteria that has been associated with multiple types of infections, including those of the eye. It has affected 68 people in 16 states, with eight of those patients reporting vision loss, four requiring enucleation (= removal of the eye, my clarification), and three dying (as of the most recent updates). A joint investigation by the US Food and Drug Administration (FDA), Centers for Disease Control and Prevention (CDC) and state and local health departments has identified artificial tears as a common exposure for many of this patient group.
In particular, EzriCare Artificial Tears, Delsam Pharma’s Artificial Tears, and Delsam Pharma’s Artificial Eye Ointment (all manufactured by Global Pharma Healthcare Private Limited) seemed to be products of concern. Throughout February, the FDA and CDC issued several warnings to both consumers and health care practitioners, cautioning them against purchasing or using these products. Global Pharma Healthcare eventually issued a voluntary recall (2). Although a recall will hopefully curb infections, the number may still rise as some of those already identified as being affected, such as Clara Olivia, who ended up losing her eye last September, were first diagnosed with a Pseudomonas aeruginosa infection as early as spring 2022 (3).
The accounts of those affected are a hard read, especially Olivia’s who, when describing her experience of the months following her enucleation, said, “I cried constantly, asking why this happened to me. How could this have happened to me? I was searching for an answer: What happened to me? At what moment? How? When? What did I do? And to not have an answer, that is the most terrible thing.” It’s clear that blame does not lie with Olivia – or any of the other patients – so what went wrong?
Although the products, which could be bought over the counter before the recall, were intended to be sterile, a number of current good manufacturing practice (GMP) violations by Global Pharma Healthcare (including a lack of appropriate microbial testing, no adequate preservative for the multi-use bottles that the drugs were distributed in, and a lack of proper controls concerning tamper-evident packaging) resulted in contaminated products. For those infected by the eye drops, the impact has been devastating – but it could have been even worse if not for the efforts of doctors, such as those at Bascom Palmer, who used photodynamic antimicrobial therapy to inhibit the bacteria when antibiotics proved unsuccessful (4).
Global Pharma Healthcare’s negligence is frustrating and scary. And it highlights the damage that can be caused – and the lives that can be lost – when corners are cut and when patient safety is not the paramount concern, especially in an era of rising antimicrobial resistance.”
The website for the company responsible for these preservative free artificial tears - which are now thankfully FDA restricted in this country, is: http://www.global-pharma.com/
To schedule an appointment with Dr. Jaccoma, call Excellent Vision at either of these two dry eye offices:
(1) 155 Griffin Rd, Portsmouth, NH 03801 (603) 574-2020
(2) 3 Woodland Rd, STE 112 Stoneham, MA 02180 (near Boston) (781) 321-6463
Do Eye Drops Cause Ringing In The Ears & Can Ringing In The Ears Mean Eye Problems?
Some online dry eye sufferers had recently asked if tinnitus (ringing in the ears) or hearing damage might be caused by Restasis (or other Cyclosporine eye drops commonly prescribed for dry eye) as the oral form of that medication has this listed as a risk factor. I decided to answer this to the best of my knowledge (the short answer is: I don’t think so – but the longer answer – along with some of my other clinical notes about Cyclosporine and an interesting association of tinnitus and another eye disease – follows.
Can Cyclosporine (Restasis, Cequa and many other iterations) cause hearing loss or ringing in the ears? While you have a Eustachian tube connecting your middle ear with the back of your throat, and a tear duct that connects your ear to the nose, I don’t believe Cyclosporine is likely to get to your ears from your eyes. Large studies under the watch of the FDA, and subsequent post-approval reporting have not listed ototoxicity (hearing/ear damage), so I see this as an additional measure of safety. The oral form of Cyclosporine can have many side effects but in the topical eye preparation, studies appear to confirm that it doesn’t get absorbed into the bloodstream, so I doubt Restasis, Cequa or the increasing iterations would cause hearing damage. Studies by Dr. Esen Akpek at Johns Hopkins’ Wilmer Eye Center: (https://www.researchgate.net/publication/291389788_Frequent_Dosing_of_Topical_Cyclosporine_A_for_Severe_Ocular_Surface_Disease) followed patients using it up to 8 times a day and their laboratory technology could not find it in their blood. Due to diversity of biology and degrees of sensitivity to medications, it is important to work with your doctors to ensure getting the best care for your health.
Interestingly, while tinnitus (ringing in the ears) is a relatively common condition, there has been a recent, small study, suggestions that it may be linked with Primary Open Angle Glaucoma (POAG, the most common kind of glaucoma). Glaucoma can lead to permanent loss of vision, so if you have tinnitus, you may wish to get checked for glaucoma, as this study found almost a 20% increased incidence of tinnitus in POAG patients: Associations between tinnitus and glaucoma suggest a common mechanism: A clinical and population-based study https://pubmed.ncbi.nlm.nih.gov/31841861/
Can you use Restasis more than twice a day? While every patient is different, the common thing about Cyclosporine is that it is (on purpose) a very weak anti-inflammatory drop. Depending on the amount of inflammation, using a weak drop twice a day may be enough - or not enough - to turn back the tide of inflammation. Meeting the amount of inflammation with the right amount of anti-inflammation, is key to overcoming the inflammation-related damage it inflicts on the ocular surface (& on the delicate tear system that is a part of that surface). Better, is to determine the cause of the inflammation and stop or reduce it so that less (or no) medication is required. The short answer is that many of my patients end up using Restasis more than twice a day. The ideal frequency will depend on the patient’s (often many) issue’s driving their dry eye disease and the goal is to reduce inflammation to the degree where less (or no) anti-inflammatory medication is required over time. Rarely do I prescribe it more than 4x/d for extended periods of time (though some do require an arsenal of anti-inflammatory products to get their eyes back to good health). As usual, consult your dry eye specialist for what is best for you.
Why does Restasis (Cequa and other Cyclosporines) sting and burn so much? Does this mean I am allergic to it or otherwise shouldn’t use it? Evaporation and dryness lead to “dry spots” (& damage) on the cornea. Corneas have more pain fibers per square inch than any other part of your body, so these dry spots can register more pain - like tiny open sores. Cyclosporine medications like Restasis are a “salty drop,” so when eyes are very dry, this can be like rubbing salt into your eye’s open sores. Fortunately, the more it works - the more you can make better tears and have a healthier cornea - and Restasis can be less uncomfortable. Once you stop Restasis it doesn’t take long for its benefits to wear off. Sadly, it can then take months for it to kick in again. Keeping these drops in the refrigerator and using them straight out of the fridge means the coolness of the drop can be more soothing than burning. Using a preservative free artificial tear 5 to 10 minutes before applying the medicated drop will often moisten and lubricate the otherwise raw surface, so there are fewer “open sores” when the salty medication is applied – and better tolerated. If eyes (and eyelids) become red and itchy while using these drops, it is possible you are developing an allergy – though eyes can become red and itchy for many reasons unrelated to medication allergies – so best to consult your dry eye specialist. An exam of the membranes under the lids and a careful history of how the problem came on, can often help sort out the cause. Sometimes more specific allergy testing is required, and it may be necessary to stop all products that come in contact with your eyes and eyelids – and then selectively adding them back one at a time over days to weeks – in order to best determine the offending cause(s).
To schedule an appointment with Dr. Jaccoma, call Excellent Vision at either of these two dry eye offices:
(1) 155 Griffin Rd, Portsmouth, NH 03801 (603) 574-2020
(2) 3 Woodland Rd, STE 112 Stoneham, MA 02180 (near Boston) (781) 321-6463
When tears don’t drain properly you get “Toxic Soup.” (and the “Toxic Soup Syndrome!”)
I should update this title to read “Are Our Eyes Living in a Toxic Soup?”
When I first posted on punctal plugs here: https://www.eyethera.com/blog/what-about-punctal-plugs-or-why-not-dam-up-those-damn-tears I alluded to the risks of “keeping the dirty bathwater in,” when punctal plugs are used to treat dry eyes. A recent publication in the Canadian Journal of Ophthalmology put a spotlight on this “Toxic Soup Syndrome” when they retrospectively reviewed cases of this, in a study published here: https://www.canadianjournalofophthalmology.ca/article/S0008-4182(23)00108-4/fulltext
Titled: “Clinical features and management of keratoconjunctivitis associated with inadequate tear drainage”
Paraphrasing their findings: The study was done by reviewing records obtained by selecting “Toxic Soup Syndrome” in an Electronic Medical Record base. 35 eyes were found to have this problem, with the majority being women at an average age of mid-sixties (ranging from the 50’s to 80’s). All patients experienced red, teary eyes and had Rosacea or meibomian gland disease. About a quarter of them had glaucoma, and a similar number developed a reduced ability to repopulate the surface corneal cells (so-called limbal stem cell deficiency - a potentially blinding eye disease). Most were using topical medications on presentation. All eyes had blocked tear drainage (in the way of “punctal plugs, cauterized puncta, or punctal and (or) canaliculus stenosis”). Treatment required stopping all preserved topical medications and using some type of anti-inflammatory therapy. Three quarters of patients improved after improvement of their tear drainage.
This type of study helps to demonstrate how important the normal “circulation” of the “lifeblood” (as tears) is to the health of the surface of the eyes. It also helps to point out how toxic typical topical medications can be (glaucoma medications being a common one - while I’ve posted on this, there is an excellent review of the “Selective Laser Trabeculoplasty” I endorse for most glaucoma patients as first-line therapy (instead of drops) from the Glaucoma Research Foundation, here: https://glaucoma.org/uk-research-study-reports-laser-based-glaucoma-treatment-is-more-successful-and-cost-effective/?gclid=Cj0KCQjwmN2iBhCrARIsAG_G2i7oVuKQ3DfAYzOTEgpFMSW_TVFv40O6pSNdYZLotkADaL1uitq2iXEaAot1EALw_wcB ). Preserved drops of every kind contain chemicals (preservatives) capable of killing - or at least inhibiting - all kinds of germs (from otherwise growing in the bottles dispensing these drops). Any chemical capable of this great feat, is also capable of hurting the tear-producing cells and glands that make our tears - so contributing to this “Toxic Soup.”
Any eyelid or tear duct problem that impairs the normal passage of tears from the eye’s surface - to the nose (I recently reviewed the “normal” pathway for tears to leave our eyes, other than pouring over the lids and down the cheeks, here: https://www.eyethera.com/blog/zmhihjvx9qfdibtgi1f2ppmkfj9fdr ) has the ability to lead to this “Toxic Soup.” Seeing an eye specialist who can diagnose and treat this problem is important to maintaining the health of your eyes - but in almost every case, prevention can be easier than the “pound of cure” that is otherwise needed once this toxic soup begins to damage the surface - and the glands supporting that surface. Healthy eyelids can make healthy tears and help keep eyes happy and healthy by providing that proper “circulation” for the surface of the eyes. Dry eye specialists can help you avoid this “Toxic Soup Syndrome!”
To schedule an appointment with Dr. Jaccoma, call Excellent Vision at either of these two dry eye offices:
(1) 155 Griffin Rd, Portsmouth, NH 03801 (603) 574-2020
(2) 3 Woodland Rd, STE 112 Stoneham, MA 02180 (near Boston) (781) 321-6463
Common Eyelid problems related to dry eye disease: Part 6b: When tears run over the eyelids (visibly crying when you don’t mean to, Part 2)
In the last post, I discussed the many, common causes of tearing when you don’t need to, try to, or mean to - best described as “reflex tearing” (apart from the babies born with teary eyes). That post includes a diagram of the anatomy, which I recommend you review if terms I use in this post are unfamiliar.
The problem when simple, reflex tearing is not the problem, usually relates to internal blockages of the plumbing itself. Of interest is the fact that in treating dry eye, we sometimes will intentionally block the plumbing with plugs (“Punctal plugs” – see my earlier post on this here: https://www.eyethera.com/blog/what-about-punctal-plugs-or-why-not-dam-up-those-damn-tears). The larger problem with a tear duct that blocks deeper in the plumbing (other than on the surface, like these plugs), is that the blockage, or “dam,” creates a pool of tears trapped in the dark recesses of that plumbing can act as food for germs – creating colonies of these microscopic critters that can back up and infect eyes, or can ooze through the plumbing and into the skin, creating infections that can be hard to treat and even life threatening, as this can function like an abscess. Antibiotics can contain some of these infections, but to get permanently rid of them, we need to fix the plumbing to “open the dam.” In the short term, this may mean an incision to drain the “abscess,” but in the longer term, it will depend on where in the system the dam occurs (and the cause of that dam).
A common cause of blockage is a “stone” – an accumulation of mucus, salts, inflammatory and infectious debris – that block the internal passages (a bit like a nose “booger” can clog up a nose). Blepharitis (especially chronic, low-grade infections), allergies and any form of dry eye disease appear to be common culprits in putting mucus, germs and inflammatory debris into tears and then into the tear ducts draining those tears. When this happens in the canaliculi (the narrow, internal passageways closest to the eyes), then even little stones can cause big troubles and may require surgical opening and removing that material with little spoons (curettes). Adding a course of antibiotics is common, as germs are often found in that mix and can be a primary cause of the stony material, as well as to complicate healing. Flushing the ducts with saline and/or cleaning solutions or antibiotics can also be helpful.
When blockages from stones, inflammation, injuries, or infections (like the dacryocystitis photo above) occur deeper in the passageways, then larger surgeries are often required – though similar flushing - as used for superficial blockages, can sometimes be helpful or even curative. When fluid “back-flushes” from the lower punctum to the upper, then we know the blockage is deeper than the “common canaliculus,” (where the two small passages come together), which means unclogging or bypassing the deeper blockage can be curative. The common non-surgical way to do this, is to either vigorously flush or probe (if possible) from the punctum to the nose, and in some cases, leave a tiny, thin, silicone tube in place to allow healing of the probed passageway to occur without healing it closed (the tube helps keep it open until it heals – typically over a few months) – or if flushing or probing is not possible due to big stones, heavy scarring or strictures – then surgery with a so called “Dacryocystorhinostomy” – or “DCR” is performed.
A DCR bypasses the blockage in the sac or duct by making a small hole in the nasal bone and connecting the tear plumbing to the nose more directly. This can be done from the outside-in (the external approach) or from the inside-out (the endoscopic, internal approach). Both approaches offer high levels of success, and the principal advantage of the internal approach is the lack of a visible scar alongside the nose. This is mostly done under general anesthesia and requires extra tools and training that is common among Ear Nose and Throat (ENT) doctors and some oculoplastic surgeons. Modern techniques rival success rates of the external approach. The external approach can sometimes offer better visibility and help in diagnosing rare causes of blockage, as from internal tumors or cysts. The external approach can be done under local anesthesia and may take a bit less time to perform. Discussion about which technique is best for an individual case is best left up to the surgeon and the patient. My personal preference is to work alongside an ENT surgeon, as I find the ENT group I work with excels at the internal approach. My years of doing external DCRs can offer some advantages in terms of probing and instilling the silicone tubing we find helps ensure best results.
More complex, is the case where the common canaliculus is blocked. This usually requires a permanent (Jones) tube be installed, to take the place of the internal natural plumbing – and this can be coupled with the DCR approach (a so-called Conjunctivo-DCR or CDCR). Oculoplastic surgeons are trained in this less common realm of subspecialty care.
So, what to do when your eyes want to cry when you don’t need or want them to? First, take care of your eyes and eyelids along the recommendations I’ve given, and most dry eye specialists agree on – and that is prevention using good lid hygiene and making your best tears. Treat infections and allergies with the help of those specialists and if common treatments for dry eye are insufficient, or tearing is frequent, then have that specialist irrigate your tear ducts to flush out debris that can contribute to clogging and to prove that your tear drainage plumbing can work properly. If there is a deeper clog, have them help you clear it without surgery, if possible, but don’t hesitate to have the surgery if your surgeon says it is indicated. Untreated, these blockages amplify reflex tearing “spill over” - which is annoying - but can lead to increasing rates and degrees of infections and antibiotic treatments can select for resistant germs over multiple recurrences. This can be a bad combination - leading to hospitalization, increasing difficulty in future surgical success and in extreme cases, risk death from aggressive, antibiotic-resistant germs.
To schedule an appointment with Dr. Jaccoma, call Excellent Vision at either of these two dry eye offices:
(1) 155 Griffin Rd, Portsmouth, NH 03801 (603) 574-2020
(2) 3 Woodland Rd, STE 112 Stoneham, MA 02180 (near Boston) (781) 321-6463
Common Eyelid problems related to dry eye disease: Part 6a: When tears run over the eyelids (visibly crying when you don’t mean to, Part 1 of 2)
I an earlier post (and what I will call “Part 1 of this discussion), I touched on “reflex tears;” https://www.eyethera.com/blog/overly-salty-tears - this is the salty tear “fire hose” we cry with when we get something in our eyes, or become emotional, or when the “sprinkler system” that makes the better, “salad dressing” tears, lets us down. Because the “fire hose” likes to run off one speed – full on – this kind of tear will commonly run over the lids and we can visibly cry. Making more and better “salad dressing” will help avoid the reflex tearing common to patients with dry eyes (most pronounced on cold, windy days, but also when we stare too long at computer screens or have air conditioning aimed at our faces). When these salty tears are blinked into our tear ducts, we can get a salty taste in the back of our throat – because that is where all our “spent tears” should go. My analogy clarifying that “circulation” is that tears are the lifeblood of the surface of our eyes – a blink is the heartbeat that refreshes or “circulates” that blood-like product over the surface and the tear ducts (located in the inner corner of our eyelids) act as the plumbing drains that connect the eye’s surface with our nose (and allows the old, used up tears a place to go, without running down our face).
Part 2 (next week’s post) is what happens when that tear duct system clogs or otherwise becomes non-functional.
But first, we need to understand that tear duct function - to understand what can make it “go wrong.”
The “Nasolacrimal Duct” or Tear Duct between the eye and the nose.
This simplified diagram shows the basic anatomy but doesn’t explain the full process. Generally, when a tear gets used up, there will be evaporation followed by some dry spots developing, that upset some of the corneal nerves and triggers a blink reflex. As the lids glide over the eye, there is a “windshield wiper-like” function that wipes the old tear towards the inner corner of the eye and brings some fresh tears up from the little “well” housed beneath the lower lid, to replace it. What happens as the lids compress and close, is that the muscles “squish” the little sac near the nose (connected to the tear plumbing), so that when the lids open, there is “suction” as the sac pops back up (a form of suction pump) – and this draws the tear into that plumbing from the little storage area in that inner corner (the lacrimal lake) of the eye. Further “pumping” of those tears will continue to “flush” the tears along the plumbing and into the nose. This helps explain the salty taste we can get from extended reflex tearing (crying) when those salty tears go down the nose, into the back of our mouth and down our throat. It can also explain the “runny nose” we can get with extended or vigorous crying.
In babies, the last portion of this system to develop is the portion of the tear duct that enters the inside of the nose. There is a small “valve” (of Hasner) that can be “stuck,” so it functions as a membrane blocking the final flow of tears into the nose. While up to 5% of kids can be born with this drainage issue, most outgrow it in the first 6 months of life, since growth of the nose will usually stretch the membrane open. Pediatric Ophthalmologists are trained to diagnose, treat, and if needed, operate on this problem when it occurs.
In my last few posts, I discussed eyelid “outties” and “innies” https://www.eyethera.com/blog/common-eyelid-problems-related-to-dry-eye-disease-part-3-ectropion & https://www.eyethera.com/blog/common-eyelid-problems-related-to-dry-eye-disease-part-4-the-eyelid-innie. When the lids turn in the wrong direction, the opening to the tear ducts can fall outside of the little well and the suction pump can be broken from displaced plumbing and displaced muscles. Irritations from lashes rubbing on the eye or from exposure of moist membranes to drying air can result in excess, reflex tearing. Exposure - like with “TED” (Thyroid Eye Disease https://www.eyethera.com/blog/8lemgnwt0bqqd15fmqr9ljrkdfe420 ) earlier posts on conjunctivochalasis https://www.eyethera.com/blog/what-is-conjunctival-chalasis-cch-and-why-should-i-care including the two followup posts, point to the pleats and folds of the normally smooth membrane that can block tear ducts, and act as a “pour spout” or “waterslide” causing diversion of tears over the lids and away from the normal plumbing. All of these issues can cause patients to present with complaints of tearing, yet each cause is different enough, so as to often require a unique approach to fix it. (I’ve addressed each of these in my earlier posts).
The problem when these are not the problem, is usually related to internal blockages of the plumbing itself. This is my Part 2 of this topic - available next week!
To schedule an appointment with Dr. Jaccoma, call Excellent Vision at either of these two dry eye offices:
(1) 155 Griffin Rd, Portsmouth, NH 03801 (603) 574-2020
(2) 3 Woodland Rd, STE 112 Stoneham, MA 02180 (near Boston) (781) 321-6463
Common Eyelid problems related to dry eye disease, Part 5: Floppy Eyelids!
When eyelids turn in the wrong direction: Floppy lids, malocclusion and snoring – a bad combination.
How can snoring be related to dry eye? - As a dry eye specialist, I can say there is a common connection. It turns out that the elastin (the tissue that gives the "elastic snap") to your voice box/airway area is the same type of elastin that is in your eyelids. If that elastin is weak, then lids lose their "snap" and can stretch out - making the lids tend to lose contact with each other when you relax (as in sleep) and they can pull away with gravity, exposing your eyes to room air (or to the ""blow-by" from a CPAP machine). Fans, Air Conditioning, or the rush of air from CPAP, (CPAP stands for Continuous Positive Airway Pressure, which is a machine that uses mild air pressure to keep breathing airways open while you sleep.) -
Image from: https://www.nhlbi.nih.gov/health/cpap illustrating (one of many options) CPAP device in use..
Image from: https://www.nhlbi.nih.gov/health/cpap
can cause increased evaporation of the tears that are exposed - and then your eyes get drier. When an eye doctor asks if you snore, they are trying to see if you might have Obstructive Sleep Apnea.
Below from the Mayo Clinic: https://www.mayoclinic.org/diseases-conditions/sleep-apnea/symptoms-causes/syc-20377631
“Obstructive sleep apnea
Above taken from the Mayo Clinic: https://www.mayoclinic.org/diseases-conditions/sleep-apnea/symptoms-causes/syc-20377631
“Enlarged image
Obstructive sleep apnea
This type of sleep apnea happens when the muscles in the back of the throat relax. These muscles support the soft palate, the triangular piece of tissue hanging from the soft palate called the uvula, the tonsils, the side walls of the throat and the tongue.
When the muscles relax, your airway narrows or closes as you breathe in. You can't get enough air, which can lower the oxygen level in your blood. Your brain senses that you can't breathe, and briefly wakes you so that you can reopen your airway. This awakening is usually so brief that you don't remember it.
You might snort, choke or gasp. This pattern can repeat itself 5 to 30 times or more each hour, all night. This makes it hard to reach the deep, restful phases of sleep.” Taken from the Mayo Clinic: https://www.mayoclinic.org/diseases-conditions/sleep-apnea/symptoms-causes/syc-20377631
________________________________________________________________________________________________
Having symptoms of drier eyes on waking can be related to loose or "Floppy" lids (as well as to sleeping with normal lids that don’t close all the way when sleeping – see my earlier post on “Mom’s eyes” in the link below). When eyelids are “too floppy” the eyelids can roll over, (or become an “outtie” – similar to the discussion on ectropion) or can “mal-occlude” – where they don’t come together well enough (and the upper lid may slide over the lower lid, creating a gap that doesn’t wet well and may result in the lashes irritating the underside of the upper lid). To determine if this may be the case, doctors need to look under the lids to test how “floppy” they are and to observe the moist membrane (conjunctiva) lining the lids (giving further clues about your eye condition).
If you snore (or suspect you snore - a spouse or significant other can help confirm it), and you are found to have floppy lids, then the "Floppy Eyelid Syndrome" seems likely related, and the doctor will commonly recommend you check with your Primary Care Physician about getting a "Sleep Study." During a sleep study, the staff will be looking for sleep apnea (described above - the condition where your airway blocks mid-snore, and you can go lengths of time not breathing). Sleep apnea has been linked to early death (heart attacks, strokes, etc.) and may contribute to ever-weakening elastin - making dry eyes worse and your life in general - quite miserable - if not shorter than it would otherwise be. Get a sleep study if your doctor recommends it (and wear the devices prescribed - like CPAP, as they can save your life). Sleep goggles, Press N Seal or Sleep Tite Sleep Rite adhesive stickers can help, as can humidifying the air in your CPAP machine, humidifying your room air and making more and better tears as I outline in earlier posts (like the “Mom’s or Dad’s eyes” post here: https://www.eyethera.com/blog/do-you-have-moms-or-dads-eyes
When lids are too “Floppy,” surgical tightening is sometimes indicated, though the above recommendations are frequently sufficient to “work-around” the problem.
To schedule an appointment with Dr. Jaccoma, call Excellent Vision at either of these two dry eye offices:
(1) 155 Griffin Rd, Portsmouth, NH 03801 (603) 574-2020
(2) 3 Woodland Rd, STE 112 Stoneham, MA 02180 (near Boston) (781) 321-6463
Common eyelid problems related to dry eye disease, Part 4: The eyelid “innie.”
Right Lower Eyelid is turning/rolling inward and putting the lashes against the white part of the eye, courtesy: eyewiki.AAO.ORG.
Part 4: When eyelids turn in the wrong direction: Entropion = turns in
https://eyewiki.aao.org/Entropion
Right Lower Eyelid is turning/rolling inward (entropion) - and putting the lashes against the white part of the eye (trichiasis).
Entropion (or inward turning lids) will result in the lashes rubbing on the conjunctival and/or corneal surfaces (called trichiasis), so that the surface can become scratched and irritated. This can be more destructive than when the lid turns out, in that continuous rubbing of lashes is a bit like adding a hairbrush to the blink. This accelerates making normally smooth conjunctival membranes red and rough, but when directed against the delicate cornea (the clear “window” of the eye) this “hairbrush” called trichiasis, can cause stronger irritations and larger, more painful scratches/abrasions. Adding the mix of germs that like to live along the base of eyelashes and the lid margin into those “open sores” is a potential recipe for disaster. As is also true for ectropion, corneas do not feel good, nor do they see well when they are dry, rough or continually scratched but can go bad in a hurry when infected.
To fix an Entropion, it is important to determine the cause, and surgery may often be required. Like ectropion, not excessively rubbing the eyes helps avoid the stretching and weakening of the ligaments that support the lid in its normal position. Weak ligaments allow the “hammock” to tip - in this case, inward. If the cause is “floppiness” (see my upcoming post on floppy eyelids and related sleep apnea), then dealing with the sleep apnea can often help stop further floppiness and may help repair it over time. When there is entropion-related lash rubbing/scratching (trichiasis), then it is common to have reflex tearing, where the “fire hose” turns on and salty water floods the eye. This is less helpful, as the salt will sting the corneal sores caused by the scratching and salt water provides little lubrication. This can break down the surface quickly and can readily lead to infections, scarring and loss of vision.
Trachoma and related eye and eyelid disease
The clinical signs of trachoma. A: Active trachoma with both follicles and intense inflammation. B: Trachomatous conjunctival scarring. C: Entropion trichiasis and corneal opacity. D: Phthisis. E: Misdirected lashes. F: Metaplastic lashes. Surv Ophthalmol. 2012 Mar; 57-341(2): 105–135.
While rare in the USA, trachoma is still the leading cause of blindness in less developed countries - and will commonly lead to the inturning of the lids - with lid, and then corneal scarring. Fortunately, if caught early, it is easily treatable with the right antibiotics and preventable with good hygiene, as it is caused by a germ that is easily spread by personal contact and is therefore very contagious. Prior surgeries, injuries (especially chemical injuries) and chronic inflammation from infections (apart from trachoma) like blepharitis (see my earlier posts on this), or allergies, can also lead to degrees of this condition. Rare immune issues like Stevens-Johnson or Ocular Cicatricial Pemphigoid, as well as some persons born with this problem, also occur.
I should mention that lashes can turn in (trichiasis) without any inturning of the lid (entropion). These misdirected lashes can have a similar effect on the surface of the eye, but most often can be managed with selective removal of these lashes (see my earlier post on this here: https://www.eyethera.com/blog/0r1w3kiho48uaz4yydxlyrogx5xksf).
Having plenty of oil and healthful tears will help to lubricate and limit the scratching and help in repairing the roughened surfaces. However, it is hard to have the good blinks eyes need, when the lashes are rubbing with each blink. Better blinking would be beneficial to making those “good tears” but is hard to do until the lid position and “blink mechanics” are restored – so fixing the lid is often required to allow proper tear production and distribution.
When entropion is related to lid spasms (as can occur after any surgery on the eye), then a temporizing injection of Botox-like medication can quell the spasming until the eye is healed and the condition may not need much more treatment. Short-term “fixes” can be as simple as adding a piece of sticky tape that splints the loose lid, or pulls the lid out and away from the eye. A mild-to-moderate, in-office treatment can sometimes be offered using special dissolvable stitches to turn the lid outward, away from the eye (called Quickert sutures). This will create a certain amount of scarring and healing that can redirect the lid forces away from the eye, but will typically wear off over time. If an entropion is severe or progresses, then more surgery is generally required and may involve tightening the lid by surgically shortening it and then resuspending it to the natural “hammock attachment sites.” Surgically “re-draping” the muscles can help rebalance the “hammock,” when just re-suspending it, isn’t enough.
Many eyelid problems will be slower to occur if the eyelids get proper support and good care over one’s lifetime. Particularly, use of toxin-containing makeup materials, or, unchecked - the overgrowth of skin germs or environmental allergies, excess eyelid rubbing or stretching - these all add up to trouble and may result in this unwanted, unhealthy eyelid (and ocular surface) condition. Getting regular eye checkups and proper eye (and eyelid) care is essential to good eye health!
To schedule an appointment with Dr. Jaccoma, call Excellent Vision at either of these two dry eye offices:
(1) 155 Griffin Rd, Portsmouth, NH 03801 (603) 574-2020
(2) 3 Woodland Rd, STE 112 Stoneham, MA 02180 (near Boston) (781) 321-6463
Common Eyelid problems related to dry eye disease, Part 3: The eyelid “outtie.”
Part 3: When eyelids turn in the wrong direction: Ectropion = turns out
Eyelids are critical to the wellbeing of the eye, as they provide the “heartbeat” that circulates the tears over the living surface of the eye, as well as protecting and supporting the eye in its socket. They are made of a tough “skeleton” (called the tarsus, or tarsal plate), with an inner lining of conjunctiva (the smooth, moist membrane that also covers the white part of the eye) and an outer layer of muscles and skin. There are tough ligaments that connect the lids to the eye socket bones at the inner and outer corners – and suspend the lids a bit like a “hammock.” Normally, the muscles controlling and supporting the lid activities of a blink, also help to “balance” that “hammock,” so it stays upright and in good alignment with the eyeball. Unfortunately, age, injury, surgeries, sun, tumors, nerve and muscle weaknesses and genetics can all contribute to an “imbalance” of the muscles, resulting in a “tipping” or turning of the “hammock.” This can lead to an outward turning (Ectropion) or inward turning (Entropion) – and each has expected (and sometimes unexpected) consequences. Below is an example of ectropion:
Involutional ectropion of the left lower eyelid. Keratinization of the palpebral conjunctiva is present. Image courtesy of Marcus M. Marcet, MD FACS. https://eyewiki.aao.org/Ectropion#:~:text=There%20are%20four%20main%20types,cicatricial%2C%20mechanical%2C%20and%20paralytic.
Ectropion (or the outward turning) of an eyelid will result in the pink, conjunctival surfaces becoming exposed to room air. This is a normally pink, moist membrane akin to the lining of your mouth. (Imagine how dry and awful your mouth could feel if you left it open all the time, so that the lining would become dry and irritated). That continuous exposure could also allow the normally moist eye membranes to become more like your skin and less like the thin, smooth, moist membrane that it should always be (this transformation to a skin-like surface is called keratinization). Skin is a rougher, drier covering – so that rough, skin-like surface could end up rubbing against the delicate cornea (the clear “window” of the eye). Corneas do not feel good, nor do they see well when they are continually scratched. The out-turning of the lid can also make it hard for the cornea to become refreshed with tears when you blink, as the tears may roll over the out-turned lid rather than be pumped up over the eye with a blink (more on this below).
To fix an Ectropion, it is important to determine the cause, and surgery may often be required. Avoiding sun damage is usually as simple as wearing sunglasses and using sunblock. Not excessively rubbing the eyes helps avoid the stretching and weakening of the ligaments. If the cause is “floppiness” (see my upcoming post on floppy eyelids and related sleep apnea), then dealing with the sleep apnea can often help stop further floppiness (and may help repair it over time).
When there is ectropion-related exposure, then having plenty of healthful tears will help to limit the dryness, exposure and scratching that is otherwise common. However, it is hard to have the good blinks which are beneficial to making good tears until the lid position and “blink mechanics” are restored – so fixing the lid is often required to allow proper tear production and distribution. Caught early, a small operation like “ignipuncture” (tiny burns applied in a precise way) can help support and turn the lid back to a normal position with the tightening from healing, caused by this procedure. In-office treatments can be offered using radio frequency technology, for that purpose. If an ectropion progresses, then more surgery is generally required and may involve tightening the lid by surgically shortening it - and then “resuspending it” to the natural “hammock attachment sites.” Surgically “re-draping” the muscles can help rebalance the “hammock,” when just re-suspending it isn’t enough.
Even a small out-turning of the inner corner of the eyelid can present a problem, as it can put the opening to the tear duct beyond the pool of old tears that would usually be drawn into the tear duct with a blink. This normal event is what allows proper turnover of the tears on the eye (remember the old, dirty, used-up tear has to be replaced by the fresh, healthy tear every time you blink. The old tear goes down the tear duct and ends up in the back part of the nose - but only if it can find its way to the opening of that tear duct. The “windshield wiper” function of the lid is also what brings the healthy tears up to replace the old tears - and a turned out lid can ruin the “wiper” function and interfere with even that level of proper “circulation.”)
The opening to the tear duct is called the punctum and once it drifts away from the eye, we call it a “punctal ectropion” and the effect can cause tears to bypass the normal tear duct and track down the inner corner of the lid. This will cause tears to run down the cheek, making it look like you’re emotionally crying. This type of tearing can also occur from blockages within the tear duct system, from loose or excess conjunctival membranes blocking the surface of the tear duct or acting as a “water slide,” diverting tears (from conjunctivochalasis - see my earlier postings on this, beginning here: https://www.eyethera.com/blog/what-is-conjunctival-chalasis-cch-and-why-should-i-care ) or from excessive “reflex tearing” caused by excessive dryness (see my post on overly salty tears and “reflex tearing” here: https://www.eyethera.com/blog/overly-salty-tears ) - so your doctor should check to find the cause of abnormal tearing and then treat it accordingly.
To schedule an appointment with Dr. Jaccoma, call Excellent Vision at either of these two dry eye offices:
(1) 155 Griffin Rd, Portsmouth, NH 03801 (603) 574-2020
(2) 3 Woodland Rd, STE 112 Stoneham, MA 02180 (near Boston) (781) 321-6463
Common eyelid problems that can relate to dry eye disease, Part 2: Say Hi to “TED.”
TED is not this patient’s real name but the acronym as described below. The rights to this photo belong to the company making the treatments described below and in this link: Tepezza
Exposure from eyelid retraction– “The Thyroid Stare” (Exposure from: Thyroid Eye Disease=TED, related to the higher levels of thyroid hormone) and/or proptosis from thyroid-related inflammation (among other inflammatory causes) behind the eye, causing eyeball “bulging.” Some unfortunate patients may have a combination, causing a high degree of eye exposure (as in the top photo before treatment, above - vs the lower above photo, after treatment) – resulting in dry eyes even when tears are otherwise good (but especially bad if the tears are “bad”). Untreated, in some cases this can lead to permanent loss of vision.
Conditions where inflammation gets behind the eye can cause the eye to be “pushed forward” - a condition called proptosis or exophthalmos, it results in the eye bulging out of the natural protection of the “bony cave” of the skull (the “orbit”) – to where the surface is exposed more than normal. This is common in Thyroid-related eye disease (TED), but can be found in other cases of genetically “shallow” orbits, inflammation, infection or from tumorous growths behind the eye(s).
If someone has TED (or any other reason for an over-exposed eyeball), then there are standard, and then newer treatments available, depending upon the degree of involvement and how much damage exists - or is at risk to exist. Job number one is to make great tears – since great tears can take good care of even very exposed eyes and bad tears can be especially bad for these eyes.
The clinical goal is to keep eyes safe and comfortable – but this can sometimes sacrifice form over function. By this, I mean that surgeries can be done to pull lids partially together (a so-called lateral and sometimes medial tarsorrhaphy) or to put a spacer into the lid to let it drop down to cover the eye better, but this may not look as cosmetically pleasing as if the eye were just to “look normal.”
This image is an example of a lateral tarsorrhaphy taken from the archives of the American Academy of Ophthalmology AAO photo and shows how the lids are brought closer together to partially cover an otherwise overly exposed eye. The cloudy, raised spot over the pupil is a corneal scar caused by excess exposure and can reduce vision in ways that is difficult to repair.
“Standard” therapy begins with all the “usual” homework for dry eye (see my earlier posts on this) and efforts to produce more and better tears as eyes bulge and exposure worsens. Adding lubricants, Autologous Serum Tears, sleep goggles and ointments at nighttime, and anti-evaporative wraparound glasses by day - can be increasingly helpful, as is true for most advanced dry eye patients. Monitoring how the inflammation and congestion behind the eye is affecting the eye-movement muscles, and the nerves involved with sensation - and particularly with vision – is key to maintaining eye health. If the eye’s health becomes compromised (double vision, pressure on the nerves, over-exposure of the eyes), then increasing levels of intervention are often required.
The common advanced interventions included steroids (prednisone) to reduce inflammation, radiation (when steroids prove insufficient or poorly tolerated) and surgeries (to decompress the swelling behind the eyes) – where bone and inflammatory tissues are removed to “make room” behind the eyes - as required to preserve eye health and function. Inflamed muscles will swell and cause poor function, resulting in double vision. Too much swelling can “pinch” the nerves, causing pain and permanent loss of vision, or cause over-exposure, causing damage to the surface of the eyes. Eventually the inflammation tends to “burn out” – so conventional wisdom was to address swelling with enough treatments to buy enough time for the inflammation to eventually subside. Smoking tobacco is like adding gas to the fire of inflammation and is strongly discouraged.
Fortunately, Tepezza is a new medication used as an infusion to fight the source of the inflammation unique to TED and has proven extremely effective against the swelling and related damage. Like most strong medications used to treat bad diseases, it can have a host of side effects that need to be weighed against the risks of the disease it is treating. These are generally manageable, but can include permanent, irreversible hearing loss in some, so proper monitoring of progress is equally important and choosing this treatment is best left to experts in the field. Dry eye doctors can help support the health of the surface of the eyes by promoting great tears and assisting in the monitoring of surface health if the disease progresses.
To schedule an appointment with Dr. Jaccoma, call Excellent Vision at either of these two dry eye offices:
155 Griffin Rd, Portsmouth, NH 03801 (603) 574-2020
3 Woodland Rd, STE 112 Stoneham, MA 02180 (near Boston) (781) 321-6463
Common eyelid problems that can relate to dry eye disease, Part 1: Bad lashes.
Trichiasis (lashes rubbing on the eye = “Bad Lashes”):
Many of us have had to pull an errant eyelash out of our eye or eyelid at some point. If the lash was totally loose and freely riding on the eye, then this is a common and “normal” occurrence, usually fixed by simple irrigation (either from tearing that washes it out, or by an eye wash rinse). But if the lash is still attached to the lid by its root, while rubbing on the eye, then this is an “abnormal” problem called trichiasis. This can be painful and in severe cases, lead to infections, scarring and loss of vision.
This condition can be a genetic, predetermined problem (often in rows of many such errant lashes) or can occur due to thinning and scarring of the lid (cicatricial), or from the more common cause relating to “Blepharitis” (see my earlier posts on this). Blepharitis can cause one or more lashes to “grow wrong” so that they turn in and rub against the eye. Sometimes just pulling the lash (epilation) and treating the blepharitis will “fix it.” Sometimes it will continue to come back the same way and need further treatment.
While treatment can vary, it is also true that the “root” (the growth “bulb”) can be quite persistent and hard to “kill.” The normal life cycle includes 3-phases of the lash, beginning with a growth phase (Anagen), a dwelling phase (Catagen) and a falling out phase (Telogen), where the lash will eventually fall out and then gradually regrow (approximately a 6 week-long cycle from start to stopping growth and then falling out). To remove a lash effectively and permanently, it is best to target it in the growth phase, when it is strongly connected to its “root.” Laser or IPL of the correct wavelength, electricity or RadioFrequency (RF) can be used to permanently “kill” a lash. Surgery can remove the lash(es) and freezing (cryosurgery) is a more destructive way to permanently remove them – though either can be extremely effective, both of these options tend to be the more painfully invasive.
Skin of color, or those with very blonde, red, white or lighter-gray lashes will generally not respond to light-related (laser or IPL) removal, as the dark skin can prevent light from penetrating deeply into the lid where the root is (essentially shielding the root from the light) and lighter colored lashes have so little “pigment” (the color of the lash) in the root, that the light doesn’t get absorbed in a way that effectively kills the root. When you have light skin and a dark lash, this can be a quick and simple treatment, with little discomfort. This is generally true for hair of all sorts, regardless of the location, and is the basic principle for all so-called “Laser Hair Removal.”
Electricity (as electrolysis) or RF (hyfurcation) are effective alternatives for permanent lash removal of any skin color and in any location. They are also most effective if done while the hair or lash is in the growth phase – or at least the dwelling phase – as once the hair or lash goes into the falling out phase, it disconnects from the root and it is often impossible to treat the root once it is “disconnected.” The principle of killing the root is common to every type of permanent hair removal and the 3-phases of hair growth accounts for the main reason it is often impossible to remove all hair/lashes with one single treatment. If the root is “missed” (due to the hair or lash being disconnected), then it will require a second (and sometimes more) attempt to permanently “remove” it. Because eyelids are sensitive and eyes are close behind the lids, it is common to have an eye doctor help you with this. In the case of electricity or RF, a small amount of numbing is common to help make the brief application of energy comfortable. An insulated “wire” is introduced alongside the lash and a brief application of current will create a burst of energy into the root. Once the lash root is sufficiently damaged, the lash becomes loose and is easily removed. If the root was effectively “killed,” then it won’t allow the lash to grow back.
Again, it may take a monthly series of such treatments to fully remove all the bad lashes, depending on which phase they are treated, how well they are treated and how many are yet to develop and become present to be treated. Uncontrolled blepharitis is also a common recipe for more to come along, so controlling blepharitis is good for the tear glands as well as for the lashes and general health of the lids, lashes, and the eye itself.
For more information on trichiasis, see also:
https://www.aao.org/eye-health/diseases/what-is-trichiasis.
https://www.reviewofophthalmology.com/article/the-annoying-lash-in-the-eye-a-review-of-trichiasis
What about Punctal Plugs (or - “Why not dam up those tears”)?
As a dry eye specialist, I often get asked about using punctal plugs for dry eye disease control. I find that the answer to that very good question is the common “it depends” - in that those with good-quality tears but poor-quantity can do well with plugs in general - but poor-quality tears generally do not.
“Punctal plugs” are anything that can block the flow of tears from reaching the usual destination involving normal, tiny openings along the inner portion of upper and lower lids, that carry tears through a drainage system that ends up in the back of the nose, leading to the back of the throat. They intentionally block this natural system, where the old, used-up tear on the surface of the eye can be blinked away and down the throat, while the new, fresh tear comes up from the little “tear gutter” (called the fornix, it is the reservoir behind the lower lid) to replace the used-up tear. If a blink is the “heartbeat” of the eye, then this turnover is the “circulatory system.”. Retaining more tear volume can work wonders for some and be problematic for others. These plugs come in many forms and sizes to accommodate the anatomic variety we see among our dry eye patients. This Mayo Clinic link provides a quick overview and diagram: https://www.mayoclinic.org/diseases-conditions/dry-eyes/multimedia/punctal-plugs/img-20007894#:~:text=One%20approach%20to%20treating%20dry,tears%20you%20may%20have%20added.
Once the common causes of inflammation have been dealt with (see my earlier posts on inflammation) - if ATD prevails, then plugs can be an eye saver (but should be periodically checked, with good lid hygiene and often replaced - to keep them from accumulating biofilm and the germs it carries – see below and my earlier posts on lid hygiene).
Treating patients, my first goal is to determine the root cause(s) of the patient’s dry eye disease. If primarily MGD (Meibomian Gland Dysfunction – where malfunctioning oil producing glands are causing dry eye disease – see my earlier posts on this), then plugs tend to be less helpful and may make things worse (more on this in a moment). ATD (Aqueous Tear Deficiency, where the “Sprinkler System” makes too little water) means the tear volume is too low (since most tear volume is made from water) and is a more common target for punctal plugging, which will retain more of that tear on the surface of the eye. Unfortunately, many dry eye patients have a mix of MGD and ATD. Poor oil will cause rapid evaporation and lead to “dry spots,” which often requires the “Fire Hose” glands to kick in, causing what we call “Reflex Tearing.” This flood leads to overflow, which can make tears run down the face even with the normal, full function of the tear drainage system. The overflow can get much worse when the system is blocked off by these plugs if reflex tearing continues after the plugs are put in.
A common cause of ATD is inflammation. If there’s a lot of inflammation, then plugs generally make it worse, as this is a “poor quality tear” that - thanks to plugging - doesn’t leave, and perpetuates the dry eye problem by leading to higher levels of inflammation. I’ve heard this referred to as “leaving the dirty bathwater in the tub and expecting it to make you clean.”
If most oil and inflammation issues are reasonably controlled and the tear volume is the remaining, primary problem, then plugs can be a great help. The types of plugging available boils down to:
- Exposed plastic (usually silicone-derived) plugs inserted directly into the “mouth” of the openings along the lid (called the punctum), which have a form of inverted umbrella design to ensure they stay in place as an anchor. The small, “contact lens-like cover” functions as an “end cap” that is visible microscopically, but rarely to the naked eye.
- “Permanent” plugs made from, small, tubular forms of plastic designed to swell inside the tiny tubes or channels that connect the punctum to the nose. These are inserted through the punctum and are carried along the channel until the swelling - or a bend in the channel - “catches” the plug and traps further flow. They are invisible but not always permanent, as they may wash through the drainage system before they “grab” and fix to the lining of the channel.
- “Temporary” plugs made from dissolvable materials designed to swell inside the tiny tubes or channels that connect the punctum to the nose. These are inserted through the punctum and are carried along the channel until the swelling - or a bend in the channel - “catches” the plug and traps further flow, but then gradually “dissolves” and re-establishes flow. The rate of dissolving is a function of the materials used to make these plugs and the amount of irritation they may cause, which can provoke faster dissolution and may lead to scarring within the channels. Like the “permanent” internal plugs, they are also invisible and can also wash through the drainage system before fixing to the wall of the channel.
- Cautery - a small burn over the mouth of the punctum, causing a scar to act as the plug. The lid is numbed before the heat is applied, so this is typically a near-painless procedure. Punctal cautery is a more “complete” plug, in that plastic plugs typically allow a little “wicking” of tears around the plug, so there can still be a little clearance.
Since tears are best when “fresh” and since plugs and cautery encourage degrees of stagnation, there are patients who get less complete benefits. Also, though tiny, exposed plugs are plastic and can be viewed as smaller “contact lenses.” That said, they, like contacts, can accumulate “plaque” (like the grunge that accumulates on teeth and acts as footing for more germs), so changing out plugs periodically (& doing good lid hygiene) is generally required. Reflex tearing is common in dry eye patients and once the plugs block drainage, the only route “out” is by evaporation, the wicking around a plug or over the lid crying, so if you puddle up in a dry wind, then consider this as a likely side effect. Seasonally the benefit of plugs depends - as those with allergies may suffer more by keeping allergens like pollen in - but drier weather like in air conditioning or winter, may be better “fits” for the plugs as dry air means more evaporative loss (as long as the occasional reflex tearing is not too great of a nuisance).
With exposed, plastic plugs, it is usually easy to remove them if problematic (not so easy if cauterized). Plugs retained along the internal channels may be forcibly flushed in a way that can propel them through the system and into the nose. Obviously, cautery means no plastic materials are involved (but also may mean more stagnation), so there’s nothing to fall out or change. Cautery should be regarded as “permanent,” although the scar will sometimes “heal open” or – in cases where the reflex tearing is problematic, may be able to be operated on to re-open (though that can be difficult or impossible in some cases). Rarely, exposed, plastic plugs can trigger scar formation that can cover over or expel the plugs and removal can be problematic, as older plugs can become more fragile and break off, leaving retained pieces inside the lower opening (which may then require a small operation to retrieve).
I've generally shied away from the dissolvable or disappearing plugs as it is hard to know when they are gone (either dissolved or having been swept away and down the tear duct into the nose or mouth). Sometimes these “internal” plugs will trap just enough stagnant tear within the channel as to provide a happy “culture medium” for germs to thrive in – and infections from these kinds of plugs can be hard to treat as this may lead to an internal abscess that then requires surgical drainage to fix.
Common dry eye treatments like lid cleaning, heated expressions and IPL are not overly likely to displace the average plug. If it falls out or dissolves, it can be easily replaced - so whether that happens from a Blephex, Lipiflow or other manipulation, I don't see that as too bad (other than cost) as it is not a bad idea to replace plugs every so often anyway (as I mentioned that they can become breeding grounds for bacteria or other grunge). As a provider of BlephEx, IPL and various heated expressions of MGD, I've not let plugs stop me from recommending that treatment if it is indicated. Fortunately, Punctal Plugs are usually covered by most insurance, are quick and generally painless to place, equally easy to remove (if exposed) and replace when indicated. Check with your dry eye specialist to see if they may be right for you.
What happens when you don’t have enough good oil and how do you fix it? (SLK, CCH and why blinking matters)…
While I’ve posted about blinks and the effect of blinking on making oil (links below), I recently was asked about SLK (and thereby CCH) – two structural eye problems which are the result of poor oil. BioTissue, among others, have dubbed this poor oil problem as “Mechanical Dry Eye” (or MDE), as friction is a driver (so a mechanical force). However, I think there is an equal contribution from the evaporation relating to lack of the “Saran Wrap-like” sealant effect of oil (so water evaporates from our tears, leaving a higher concentration of salt to cause more surface damage and leads to inflammation. Inflammation added to friction “unpeels” the glue and fibers that hold the conjunctival membrane to the underlying white of the eye (or sclera), allowing it to “come loose.” Further friction leads to more inflammation and the vicious cycle perpetuates dry eye and related surface eye diseases.
SLK (superior limbic keratoconjunctivitis) is essentially the same as CCH (conjunctivochalasis) - both are when the conjunctival membrane "comes loose" and develops pleats and folds that interfere with the proper eyelid “squeegee” of tear flow over the eye, as well as causing friction-related irritation. Instead of affecting the lower part of the eye like CCH, SLK affects the upper. Surprisingly it appears to be less common than CCH, possibly because the inflammatory tear products are in greater contact with the lower lid from gravity, possibly because our eyes more commonly track downwards rather than upwards – possibly due to the differences of the mechanical forces relating to the difference in the size and position of the upper vs lower lids -but the effect of friction and inflammation on the conjunctival membrane is the same. It also appears more common in Thyroid-related eye disease and Rheumatoid Arthritis, but then so is my perception of CCH, too.
An autograft (where a portion of conjunctiva harvested from another area and “transplanted” to cover the area exposed when the damaged conjunctiva is removed) - or the amnion surgery used by some in CCH repair (where a piece of amnion is glued or sutured over the exposed area) can work - but I found that radio frequency (RF) works great for both CCH and SLK - and offers the opportunity to do an (off label) RF-heated expression of the clogged MGs that appear common to causing both SLK and CCH. In the past, Silver Nitrate (on a wooden stick applicator) was also used to treat SLK - but it causes a chemical burn rather than an electrocautery or RF-plication "singe" - so I didn't find it better (as it seemed less predictable and doesn't fix the problem - obstructive MGD - causing the problem – SLK as we can with RF).
For more on CCH, see these earlier posts: https://www.eyethera.com/blog/what-is-conjunctival-chalasis-cch-and-why-should-i-care and for some embedded links to see how I actually do my treatments (and a study I published on the success of these treatments), see:
https://www.eyethera.com/blog/conjunctival-chalasis-cch-part-2-how-do-we-fix-it
Lastly:
https://www.eyethera.com/blog/cch-part-3-when-do-we-treat-cch-and-what-are-the-options
Early in my career, when I began to specialize more fully in all things related to dry eye disease, I had the good fortune to spend some time with a true giant in that specialty (Dr. Donald Korb – inventor of Lipiflow). Due to his influence, I became one of the first doctors to offer Lipiview and Lipiflow north of Boston (where Dr. Korb invented it). I gained a huge appreciation for the variety of blinks and blinkers (Lipiview was the first commercial technology to monitor blinks). My experience is that those with uniformly poor blinks tended to have worse MGD (dysfunction of the oil producing glands of the eyelids) and those fortunate few who had better blinks tended to have less MGD.
As a fellow partial blinker, I can relate to how confusing this is. I see it as a measure of higher IQ (since I have the same issue;) but I believe it boils down to the fact that nobody teaches us how to blink, so some (perhaps most) of us learn these “bad blinks.” As children we had perfect eyes and perfect tears - so we hardly had to blink. As we “grow up” we don’t do ourselves any favors by partial blinking. Digital devices add to partial blinking by staring and then stagnating oils. I’ve posted on some of this stuff here:
https://www.eyethera.com/.../how-important-is-oil-to-our... and
https://www.eyethera.com/.../why-do-my-oil-supplements...
Here, I offer some tips on how to remedy our “bad blink habits:”
and
https://www.eyethera.com/blog/avoiding-a-heart-attack-on-the-surface-of-your-eye
Probably the best way to deal with this issue is prevention through education. Helping our children develop good habits - working on better blinks, encouraging more time spent outside where natural stimulation from wind and sun can help promote good blink habits (and hopefully less time spent on digital devices - or at least following the 20/20/20 rule), good diet and exercise programs - and proper lid hygiene. Add to that regular eye checkups that can include monitoring the health of our tears and the surface of the eyes.
Some years ago, I had the good fortune to come across a European PhD candidate who was focused on these blink issues and he produced a useful website you can visit here:
https://www.blinkingmatters.com/
Sjogren’s Disease: Autoimmune dry eye Part 5
The key question asked of Sjogren’s researchers is – “what does the future look like for Sjogren’s patients?” Fortunately, there are new consortiums of research activities that appear to bode well for a good answer.
Is a consortium of private corporations and government institutions structured to help understand and accelerate treatments for certain autoimmune diseases (Rheumatoid Arthritis and Lupus in particular) that are related to Sjogren’s Disease in some subsets of patients. Founded in 2014, there has been a lot of activity which is slated to continue over at least the next 4 years.
From their website, we find this:
“AMP-AIM” is a next-level evolution of the AMP program. From their website:
https://fnih.org/our-programs/AMP/autoimmune-and-immune-mediated-diseases
“As a next step, AMP AIM is working to refine and extend the single-cell analysis of biopsy (e.g., synovium, kidney, skin, salivary glands) and blood samples to include additional diseases, including psoriasis/psoriatic arthritis and Sjögren’s disease.” Finally, Sjogren’s Disease is getting the much needed spotlight it deserves from a consortium of heavy hitters who are in a great position to figure it out and effectively treat it!!
Dr. Nancy McNamara is an optometrist working at UCSF who notes that the cornea has the most number of nerves per square inch of any portion of the human body, so it perhaps no surprise that it can “hurt” even when we can’t clinically find anything out of place using conventional examination methods (the so-called “pain without stain”). Lacritin is a naturally occurring compound found in tears, which has a profound impact on restoring corneal nerves and the surface cells lining the cornea (epithelial cells). Measuring the amount in tears can help to increase our ability to find Sjogren’s patients, as they commonly have very low values of this compound. Equally exciting is the likelihood of soon treating eyes with extracts of this compound - a product called “Lacripep” (which is a smaller, active ingredient in Lacritin). Of a side interest to me, the company making this product is based in Charlottesville, VA (my Ophthalmology Residency alma mater). A recent study can be found here: https://journals.lww.com/corneajrnl/Fulltext/9900/Lacripep_for_the_Treatment_of_Primary.84.aspx
Dr. Anat Galor is an Ophthalmologist working out of the University of Miami, Bascom Palmer Eye Institute. She headed a small study looking into fecal microbial transfer from healthy donors to the gut of active Sjogren’s patients. Unfortunately, these transfers did not “take” long enough to have a significant impact on the receiving patient’s gut to show significant benefits, but there was enough promising data to turn attention towards a “customized biome transfer,” where needy patients could have pills tailored to the more precise germs required to “fix” their gut-related autoimmunity issues. She also pointed to the promising research using natural anti-autoimmune injections of intravenous immunoglobulins (IVIG) to help with the “pain without stain” corneal nerve pain – so a possible adjunct to the Lacripep treatments mentioned earlier.
Dr. Vidya Sankar referenced the possibility of gene therapy, as this has been increasing used for other diseases and the ability of targeting the diseases salivary glands (and perhaps the tear glands) seems within reach. Regenerative therapies are mostly available only in the form of Autologous Serum Tears for affected eyes currently, but this area appears likely to bear more fruit for our Sjogren’s patients sooner than later. Oxervate is a form of Neurotrophic Growth Factor that is already available to treat damaged corneal nerves and is in studies alongside Lacripep, to see if they can be used in this regenerative way. Neurostimulation with the nasal spray in Tyrvaya, is also under study as it may work in a similar way – but without having to add more drops directly to the surface of the eye.
In my earlier posts, I covered much of what is already available for advanced dry eye treatments common to the care of Sjogren’s patients:
https://www.eyethera.com/blog/segment-10-aampb-what-we-know-about-inflammation
https://www.eyethera.com/blog/segment-10-b-when-we-are-at-war-with-ourselves
https://www.eyethera.com/blog/not-so-secret-weapon-of-dry-eye-treatment-intense-pulsed-light-or-ipl
https://www.eyethera.com/blog/ive-tried-everything-now-what